Pregnancy Changes and Discomforts
Pregnancy is a time of change for everyone - mother, baby, partner and your relationships.1 From the time of conception to the birth of your baby, your body will go through an exciting transformation.1 This webpage describes normal changes during pregnancy and ways to manage any related discomforts.
To learn more about concerning symptoms that you should speak with your healthcare provider about, please go to our Complications webpage.
Physical Changes
Along with your expanding uterus, changing hormone levels are responsible for many of the physical and emotional changes that you experience during pregnancy.1
- Human chorionic gonadotropin (hCG) is also called the "pregnancy hormone". It is the one which confirms pregnancy in early pregnancy tests. HCG is produced by the placenta and nausea is related to this hormone.1 4
- Progesterone is produced firstly by the ovaries and then by the placenta starting in the second trimester. Progesterone keeps the placenta functioning properly and the uterine lining healthy and stimulates the growth of breast tissue. Heartburn, acid reflux, and indigestion are related to high levels which relaxes the stomach and bowels to increase absorption of nutrients. This hormone relaxes the uterus and prevents it from contracting too much during pregnancy.1 4
- Estrogen is the hormone responsible for making the uterus grow and increasing its blood supply throughout pregnancy. It also increases vaginal mucous production and stimulates the development of breast ducts in preparation for breastfeeding.1 4
- Relaxin is the hormone that relaxes and softens ligaments and cartilage in the body during pregnancy, including the cervix. This helps with expansion of the pelvic joints during labour and birth, to allow the baby to move through the birth canal more easily.1 4
- Oxytocin causes the uterus to contract during labour. It stimulates uterine contractions after the baby is born in order to assist with the delivery of the placenta, close off the blood vessels that were attached to it, and begin to shrink the uterus back to its original size. Oxytocin is also responsible for stimulating your breastmilk to flow. This is known as milk ejection reflex (MER), and it also supports bonding and attachment.1 4
1st Trimester:
The first trimester is from conception to the end of the 12th week of pregnancy. Although you may not look pregnant during the first trimester, your body is going through enormous changes. In the first few weeks following conception, your hormone levels change significantly. Your uterus begins to support the growth of your placenta and fetus, your heart rate increases and your body adds to its blood supply to carry oxygen and nutrients to your developing baby.4
Nausea and Vomiting:1 4
One of the most common discomforts of early pregnancy is nausea and vomiting affecting up to 85 percent of all pregnant women. Also known as morning sickness, it can occur at any time of the day. It generally starts between the fourth and ninth weeks of pregnancy and subsides by sixteen weeks. Nausea is related to the increased production of pregnancy hormones. Once your body adjusts to the new levels, your nausea subsides. However, some women may experience more severe symptoms for a longer period of time. It is important to talk to your healthcare provider for tips about managing nausea and vomiting. For severe cases of nausea, there is medication which is safe to use during pregnancy. Some helpful tips include:
- Eating a few crackers or dry toast (especially before getting out of bed in the morning).
- Getting out of bed or up from a chair slowly and avoiding sudden changes in position.
- Eating a snack such as nuts, yogurt, and cheese before bedtime.
- Eating small, light, frequent meals or snacks before feeling hungry so your stomach does not feel empty.
- Eating foods that appeal to you.
- Avoiding spicy, fried, or fatty foods.
- Choosing cold, acidic beverages (e.g., lemonade) or aromatic beverages (e.g., mint or orange herbal tea).
- Avoiding strong odours, heat, humidity or noise.
- Drinking small amounts of fluid during the day between meals instead of while eating.
- Using acupressure wristbands marketed for motion sickness.
- Making sure you get enough sleep.
- Getting help and support from friends and family.
- Taking ginger in forms such as lozenges or drinks. It is best to avoid ginger in large quantities or in tablets since few studies have been conducted thus far to establish the safety and efficacy of this food.
- Vitamin B6 (pyridoxine) may be used in consultation with your healthcare provider. Studies have shown its probably effective at reducing nausea without side effects. It is not effective for vomiting.
Breast Changes:4
Soon after conception, hormonal changes may make your breasts tender, fuller, sensitive, or sore. Breasts develop and enlarge under the influence of estrogen, progesterone and prolactin. The breast changes during pregnancy occur as the milk ducts are growing in preparation for breastfeeding. Your increased blood supply during pregnancy also makes the veins in your breasts become more noticeable. By about 12 weeks of pregnancy, the skin of your nipple and areola may start to darken. Skin colour changes are very individual to each woman. Women with darker hair and darker complexions tend to notice more colour change than fair-skinned women. Your nipples may become more prominent and feel quite sensitive or even sore. Some helpful tips include:
- Wearing a good-quality support bra or a sports bra.
- Wearing a bra without underwire.
- Wearing a bra while sleeping to support the changing breasts.
Fatigue:1 4
During the first few months of pregnancy, you may feel very tired. Don’t worry - it’s normal to feel this way. The increased levels of progesterone can make you feel more sleepy. Your metabolism also increases, and this consumes a lot more of your energy. Some helpful tips include:
- Paying attention to your body and resting or taking naps as needed.
- At work, finding a quiet place to close your eyes and relax.
- Accepting help from your partner, family and friends.
- Eating small amounts of food many times during the day. Use Canada’s Food Guide for examples or go to Eating for a Healthy Pregnancy page.
- Drinking plenty of water.
Frequent Urination:1 4
Frequent urination is a normal change caused by the growing uterus putting pressure on your bladder and the kidneys which causes an increased production of urine. This pressure may cause you to leak urine when you cough or sneeze. When the baby drops or engages into the pelvis as labour is approaching, you will have more frequent urination. If you feel any pain or burning when you urinate, you may have an infection and should speak to your healthcare provider. Some helpful tips include:
- Drinking less in the evening.
- Going to the bathroom every time you feel an urge to urinate.
- Making sure your bladder empties completely.
- Sit comfortably on the toilet relaxing legs and knees. Keep legs apart not together. Do not strain to urinate but let it flow out easily.
- When you think you are finished bend forward and a little more may come out. This may become more difficult as your abdomen grows so try just small rocking movements.
- Requesting a referral to a physiotherapist that deals with pelvic floor issues.
- Doing Kegel exercises.
Kegel exercises provide strength training for the muscles that surround your pelvic floor. Doing a series of Kegel exercises several times a day will strengthen the muscles that stretch during childbirth and may prevent stress incontinence (urine leaking when you cough, sneeze, or laugh). These exercises can be done in any position. To do a Kegel exercise, imagine you are trying to hold back urine and squeeze the muscles that you would use to do that. You can also describe it as sucking fluid through a straw. Don’t hold your breath or tighten your stomach or buttocks. Hold for about 10 seconds. (If you are not able to hold for 10 seconds, work your way up to it over several days or weeks.) Repeat the squeeze-hold-relax routine 12-20 times.2
Feeling Faint, Lightheaded, or Dizzy:1 4
Feeling faint, lightheaded, or dizzy during early and middle pregnancy is common. This feeling is related to your higher hormone progesterone levels which relax the walls of the blood vessel, lowering blood pressure. Low blood sugar or iron levels may also contribute to this. Some helpful tips include:
- Slowly getting up from a sitting or lying position.
- Eating small frequent, nutritious snacks throughout the day.
- Eating iron‐rich foods.
- If you feel faint:
- Sitting down and putting your head between your knees.
- Loosening tight clothing.
- Asking someone to bring you a cool cloth to put on your forehead or back of your neck.
- Contacting your healthcare provider if the feeling does not go away.
Increased Vaginal Discharge:4
Increased vaginal discharge is a normal part of pregnancy. Normal vaginal discharge during pregnancy is called leukorrhea, which is thin, white, milky, and mild smelling. If the discharge has an odour, is green or yellow, or there is pain, itching, or soreness in the vaginal area, you should consult your healthcare provider for assessment. Some helpful tips include:
- Wearing breathable, unscented panty liners.
- Notifying your healthcare provider of any changes in vaginal discharge.
2nd Trimester:
By the middle part of pregnancy, most women begin to feel more energetic and more settled. You will also notice that your body’s shape and size will begin to change.
The second trimester of pregnancy (from week 13 to week 27) is the time when most women start to look and feel pregnant. By 16 weeks, the top of the uterus (called the fundus), will be about halfway between your pubic bone and navel. By 27 weeks with a single pregnancy, the fundus will be about 5 cm (2 in) or more above your navel. Some women may find that the second trimester is the easiest part of pregnancy. The placenta, which has been developing in the uterus, has taken over most of the hormone production and the hormone levels begin to even out. For some women, the breast tenderness, nausea and vomiting, and fatigue of the first trimester ease up or disappear during the second trimester, while the physical discomforts of late pregnancy have yet to start.
Skin Changes:1 4
Melasma (also known as chloasma) is the darkening of the skin on your forehead and cheeks (looking somewhat like a mask). Development of the linea nigra, which is a dark line from your navel all the way down your abdomen, is also common, as well as darkening of the nipple and areola tissue. Stretch marks called striae may also develop around your abdomen and other parts of your body. There is no way to prevent stretch marks. The degree to which you develop stretch marks is determined genetically. Due to hormonal changes in pregnancy, dry and itchy skin is common. Some helpful tips include:
- Soaking in oatmeal baths.
- Applying cool compresses.
- Avoiding harsh soaps and bathing in hot water.
- Consulting with your healthcare provider about medications that are safe to prevent itching.
- Practicing sun safety guidelines, including use of sunscreen, wearing a hat, and covering skin when outdoors.
Breasts:1 4
Your breasts may not be as tender as they were in the first trimester, but they will continue to grow and prepare for breastfeeding. By about mid-pregnancy, under the combined effects of many hormones, yellowish or clear breastmilk called colostrum is produced. It may leak from your nipples from this point on. Colostrum will be the first breastmilk your baby receives shortly after birth. It’s high in nutrients and antibodies. The amount of colostrum leakage varies from woman to woman. This does not affect the success of breastfeeding. Some helpful tips include:
- Wearing a good-quality support bra or a sports bra with no wires.
- Increasing bra size.
- Wearing breast pads if breasts are leaking and changing them when wet.
Back and Ligament Pain:1 4
A number of factors can contribute to ligament and back pain during pregnancy. These include:
- Your growing baby will cause you to lean back to find your center of gravity, which can cause strain on your lower back.
- The hormone relaxin softens ligaments and cartilage in the body during pregnancy, including the cervix. It is responsible for expansion of the pelvic joints during labour and birth to allow the baby to move through the birth canal more easily.
- Ligament pain when walking is caused by stretching of the ligaments supporting the uterus as it adjusts to its increasing size and weight.
One of the benefits of physical activity during pregnancy is that it can decrease this pain, especially in the lower back. The Canadian guidelines for physical activity throughout pregnancy recommend 150 minutes of moderate-intensity physical activity over at least 3 days each week. Even better, be active every day. Some helpful tips include:
- Using good posture.
- Using a cushion for back support.
- Avoiding wearing high-heeled shoes.
- Wearing low-heeled (not flat) shoes with good arch support.
- Using good body mechanics. To lift something from the floor, place feet hip-distance apart, bend knees with the back straight, keep the load close to your body at waist level and do not twist/rotate.
- Avoiding heavy lifting when possible.
- Limiting standing for long periods of time. Keep weight equal to both legs (not shifted to one leg).
- Accessing services such as a massage therapist or physiotherapist.
- Using relaxation, yoga, and/or stretching exercises.
- Practicing pelvic rocking (tilts) to keep the spine flexible (flatten your lower back by pulling in your stomach and buttocks).
Constipation:4
Constipation is common during pregnancy as food moves more slowly through your bowels. It affects up to 50 percent of pregnant women. Taking iron supplements can also cause constipation and black stool. It is most often observed in the first and third trimesters.
Symptoms of constipation include:
- Abnormal consistency of stool (stool too hard and dry).
- Decreased amount of stool or frequency of bowel movements (less than three times per week).
- Difficulty moving the stool out.
Some helpful tips include:
- Drinking plenty of fluids (aim for 2.3 L or 9.5 cups of water per day).
- Eating high-fibre foods. Foods high in fibre include ground flaxseed, fresh fruits and vegetables, whole-grain breads and cereals.
- Engaging in moderate-intensity physical activity such as walking or swimming.
Hemorrhoids:4
Hemorrhoids are dilated veins that form in the wall of your rectum and anus. They can be caused by constipation and increased pressure on the rectal veins during pregnancy. Hemorrhoids have no negative effects on your health or your unborn baby, but they are uncomfortable.
Symptoms of hemorrhoids include:
- Pain, inflammation, burning or itching in the anal area.
- Minor bleeding with bowel movements.
Some helpful tips include:
- Cleaning the anal area thoroughly after each bowel movement.
- Having a warm sitz bath three to four times a day for 15 – 20 minutes.
- Consulting with your healthcare provider about applying hemorrhoid cream or ointment locally as this may help to reduce the symptoms of hemorrhoids.
Inflamed or Bleeding Gums:1 4
Dental care during pregnancy is an important part of overall health care. During pregnancy, the gums naturally become more swollen and may bleed after brushing. Hormonal changes during pregnancy can increase the risk of developing periodontal (gum) disease. Poor oral health may also affect the health of your developing baby. Some helpful tips include:
- Avoiding soft, sweet, and sticky snacks that are high in carbohydrates and sugar.
- Cleaning your teeth after snacking to prevent cavities.
- After vomiting, rinsing your mouth with water or with fluoride mouthwash as soon as possible.
- Brushing your teeth at least twice a day using a soft toothbrush with fluoride toothpaste.
- Flossing regularly.
Pregnant women with periodontal disease may have a higher risk of having a preterm or low-birth-weight baby. Continue your regular dental checkups and cleanings by a dental professional to detect and prevent periodontal disease.
Leg Cramps:4
Up to 30 percent of women can be affected by leg cramps during pregnancy. The cause of leg cramps during pregnancy is not fully known, but they may be caused by reduced levels of calcium or increased levels of phosphorus in the blood. Leg cramps are more common in the second and third trimesters of pregnancy and happen most often at night. Some helpful tips include:
- Passive stretching and massaging the affected muscle which will help ease the pain of an acute attack (e.g., for calf cramping – straighten the leg while pointing your toes up towards the ankle or heel walk until the pain resolves).
- Regular stretching of the calf muscles throughout the day.
- Walking to stretch the calf.
- Placing a pillow at the end of the bed to avoid stretching out leg during sleep.
- If leg cramps are in one leg only and there are signs of swelling and redness of the leg, it is possible that there might be a blood clot present. Consult with your healthcare provider.
Nasal Congestion:1 4
Pregnant women experience nasal stuffiness due to estrogen causing an increased production of mucus. The safest treatment of these symptoms is a saline nasal spray. Ways to prevent nasal congestion include:
- Refraining from smoking as well as avoiding second-hand and third-hand smoke.
- Avoiding antihistamines unless recommended by your healthcare provider.
Some helpful tips include:
- Placing warm, moist towels on your face.
- Breathing steam from a hot shower or a pot of boiling water.
- Using a cool mist humidifier.
- Massaging your sinuses by rubbing on the bony ridge above and under the eyebrows, under the eyes, and down the sides of the nose.
- Drinking water.
- Using saltwater nose drops made from 1/4 teaspoon of salt dissolved in one cup of warm water or over-the-counter saline drops.
- Nosebleeds can also happen more frequently, especially in the winter when the air is dry. A humidifier may help to prevent them.
Quickening (first fetal movement):4
Quickening or first perception of fetal movement varies considerably among pregnant women. It is generally experienced between 16 and 20 weeks of gestation. In your first pregnancy, this can occur around 18 weeks’ gestation and in following pregnancies it can occur as early as 15 to 16 weeks’ gestation. Early fetal movement is felt most commonly when you are sitting or lying quietly and concentrating on your body. It is usually described as a tickle or feathery feeling below the umbilical area (belly button). Sometimes the movement of the fetus is not felt as quickly if the placenta is on the front wall of the uterus. As the fetus grows larger, the feeling of fetal movement becomes stronger, regular, and easier to detect.
Once you are aware of fetal movements you should be able to notice at least six fetal movements in two hours. If you notice a change or decrease in the usual fetal movements, contact your healthcare provider.
3rd Trimester:
In the third trimester, which is from 28 weeks’ gestation until birth, many women will begin to feel uncomfortable and tired as their baby grows in size placing pressure on the internal organs, including the lungs and bladder. It is also the time when changes occur in preparation for labour, birth, and breastfeeding. Hormonal changes cause the cervix to soften and the uterus to become more responsive to oxytocin, which stimulates contractions and initiates labour.
Fatigue/Sleep Disturbances:4
The third trimester is a time to expect increasing insomnia and night waking. Strange dreams are also common in the last few weeks of pregnancy. The need to take daily naps returns as the due date approaches. Insomnia is one of the most common sleep disorders for pregnant women.
Symptoms of insomnia include:
- Difficulty falling asleep.
- Frequent night waking.
- Early waking.
- Variable sleep quality (i.e., several nights of poor-quality sleep followed by a night of good-quality sleep).
- Fatigue or sleepiness during the day.
- Difficulty concentrating.
- Forgetfulness.
- Irritability.
- Decreased level of motivation or energy.
- Concern about amount and quality of sleep.
Some helpful tips include:
- Sleeping as long as necessary to feel rested.
- Keeping regular sleep hours such as going to bed and waking up at the same time every day.
- Avoiding stimulants (e.g., coffee; chocolate; caffeinated, carbonated beverages), especially in the hours before bedtime.
- Creating an environment conducive to sleep (e.g., turn off inside and outside lights and electronic devices, control surrounding noise and temperature).
- Avoiding use of the bedroom for non-sleep-related activities (e.g., studying, eating).
- Resolving problems and daily concerns before bedtime or making a list of these for the next day.
- Incorporating regular physical activity into the day, preferably more than four hours before bedtime.
- You should avoid self-medication to assist with sleep issues and always consult your healthcare provider before taking any over-the-counter, prescription, or natural sleep aid.
Frequent Urination: see 1st trimester
Braxton Hicks Contractions:1 4
Braxton Hicks contractions are contractions of your uterus that occur during the third trimester of pregnancy. Sometimes, Braxton Hicks contractions have been referred to as false labour. They are perfectly normal. In some women, they occur as early as the second trimester. Common events can sometimes trigger Braxton Hicks contractions, such as increased activity, you or baby, touching your abdomen, dehydration, sexual intercourse, or having a full bladder.
Braxton Hicks contractions become more obvious and frequent as the pregnancy progresses occurring several times an hour and/or several times a day and do not lead to cervical changes. Although these contractions are pain-free in the majority of women, painful Braxton Hicks contractions have been reported in some cases.
For more information about how prelabour contractions differ from true labour contractions, visit How do I know if it is true labour?
Some helpful tips include:
- Changing positions such as taking a walk or lying down.
- Drinking a glass of water.
- Practicing relaxation exercises such as deep breathing or meditation.
- Eating a snack.
- Having a warm bath.
Note: If you are unsure about your contractions you should contact your healthcare provider to rule out preterm labour.
Shortness of Breath:4
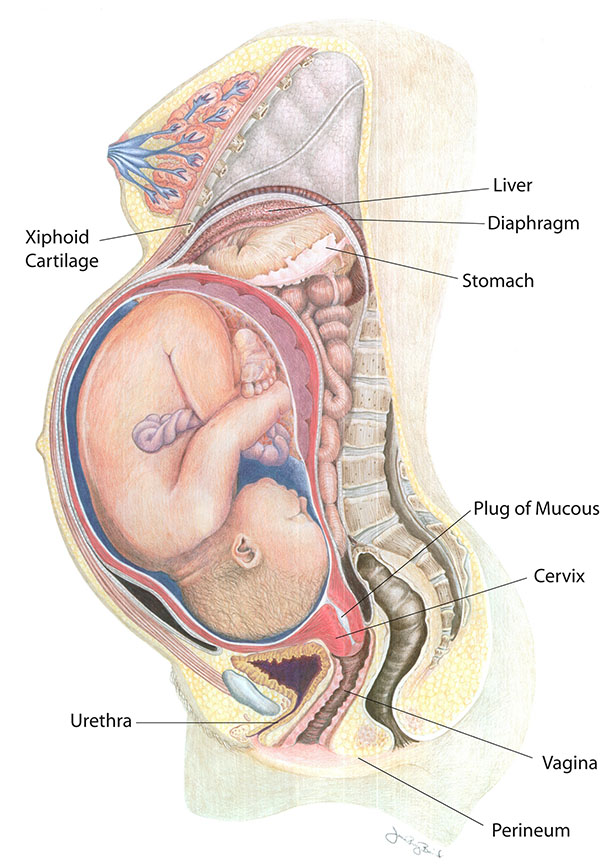
Shortness of breath is a common complaint in pregnancy. In the last trimester of pregnancy, the expanding uterus pushes up against your diaphragm resulting in shallow breathing. Near the end of pregnancy, when the baby engages, many women will feel less shortness of breath as there is more room for the lungs to expand once the baby drops deeper into your pelvis. Some helpful tips include:
- Practicing good posture.
- Exercising daily.
- Avoiding overly strenuous activity.
- Relaxing.
Faster Heart Beat and Breathing:4
By the end of your pregnancy your blood volume will increase by 30-50% to support your growing placenta. As a result, your heart rate increases by 10-15 beats per minute to provide additional oxygen and nutrients to your baby. Your body requires more oxygen so you will notice that you breathe faster and deeper and may feel breathless at times. Some helpful tips include:
- Listening to your body and taking frequent rest periods.
Indigestion and Heartburn:4
Indigestion and heartburn (acid reflux) occur when the contents of your stomach rise back up into your throat or mouth. Since stomach contents are acidic, reflux causes a burning sensation in your stomach and a taste of acid in your throat. The decreased tone at the opening to your stomach because of increased levels of progesterone, and the pressure of your uterus are factors that contribute to reflux. This affects approximately 30% to 80% of pregnant women.
Symptoms of gastroesophageal reflux, which often appear after a meal, include:
- Burning sensation in the stomach.
- Pain in the upper abdomen.
- Regurgitation.
- Acidic or bitter taste in the throat.
- Indigestion.
- Nausea and vomiting.
Some helpful tips include:
- Elevating your head 10 cm to 15 cm off the bed (using pillows) so that your head and shoulders are higher than your stomach (gravity will help prevent reflux).
- Avoiding lying down after eating.
- Eating small, light, frequent meals (e.g., every two to three hours).
- Avoiding foods/drinks that promote reflux such as coffee, tea, chocolate, carbonated beverages, mint, fatty, or spicy foods.
- Avoiding eating or drinking before bedtime.
- Chewing gum to increase saliva production (this can help neutralize gastric acid).
- Avoiding clothes that are too tight as they may put pressure on the abdomen.
- Eating smaller amounts more often during the day and do not drink fluids with meals, but 20-30 minutes after.
If these measures don’t help, consult your healthcare provider before taking any over-the-counter medication. Prescription medication may also be an option.
Varicose Veins:4
Varicose veins are more common as women age; weight gain, the pressure on veins returning blood from your legs, and a family history increase the risk of developing varicose veins during pregnancy. Varicose veins can occur in the legs, vulva, and anus (hemorrhoids). Some helpful tips include:
- Avoiding standing for long periods of time.
- Avoiding sitting with legs crossed.
- Gaining weight within the recommended limits.
- Elevating legs whenever possible.
- Using support hose following discussion about sizing with her healthcare provider. The cost of these may be covered by supplementary health benefits.
- Sleeping with legs elevated.
- Exercising to improve circulation.
Lightening:4
Your breathing improves by the end of the third trimester as your baby drops into position in preparation for birth. This is often a relief to many women; however, you may notice that you feel the urge to urinate much more frequently as the baby is lying low on your bladder.
Healthy Weight gain:
It is important for women to gain the recommended amount of weight to have the healthiest pregnancy possible. For more information, go to our Healthy Weight Gain During Pregnancy webpage.
Emotional Changes:1
Pregnancy is a time of transition and preparation. Your body, as well as your perspective on life is changing. Some questions you may be asking yourself may include: How is this baby going to change our relationship and our life? What kind of parent will I be? Why am I happy one minute and crying the next?
- Your mood swings are directly related to your changing hormone levels. Mood swings are common during the first trimester (6th-10th week) and then again in the third trimester.
- While heightened emotions are normal in pregnancy, there may be times when they interfere with your daily life and relationships. If you feel this way, talk to your healthcare provider about these feelings.
- It is also important to remember that symptoms of depression are often confused with common pregnancy symptoms. For example, sleep disturbances, loss of appetite, and difficulty concentrating may be signs of prenatal anxiety and depression.
- About 10% of pregnant women require some type of assistance for prenatal depression and anxiety.
- Go to Perinatal Mental Health for more information.
- Some tips for taking care of your emotional health during pregnancy include:
- Staying active. Exercising not only helps with mood but is a good way to manage stress.
- Eating well, including good sources of Omega-3.
- Taking time to relax and rest whenever possible.
- Avoiding stressful situations and people.
- Sharing your thoughts and feelings with someone you trust.
- Being honest with your healthcare provider about your feelings throughout your pregnancy.
Changes for the Partner:1
Waiting for parenthood is an emotional experience. At times you may feel excited, proud and confident, while at other times you feel helpless and uncertain about the future. It is important to talk to your pregnant partner or your close friends and family about these changes to your life and relationships.
During the pregnancy, partners may:3
- Feel a loss of freedom and increased sense of responsibility.
- Think about life, immortality, and pride at continuing the family for another generation.
- Evaluate their job and financial situation.
- Become protective of their pregnant partner.
- Feel “left out” and not part of the pregnancy.
- Feel anxious or worried about their role during labour and birth.
- Experience “sympathy” discomforts (Couvade Syndrome) e.g., weight gain, cravings, nausea, backaches, etc.
- Feel that their pregnant partner is less available to them emotionally, physically, and sexually.
Sex and Pregnancy
As your body changes and grows throughout pregnancy you may notice a change in your sexual desires and sexual relationship with your partner. This is normal. Learn more about sex and pregnancy.

Adapted / Reproduced with permission from Best Start by Health Nexus.
Last modified on: August 16, 2019
References
http://www.beststart.org/resources/rep_health/index.html
http://www.ontarioprenataleducation.ca/physical-changes/